Sleep Disorder Drains UK Economy of Billions in Lost Productivity
British businesses are facing a staggering annual productivity loss exceeding £4 billion due to a common but frequently undiagnosed sleep condition affecting millions of workers nationwide. Obstructive sleep apnoea (OSA), which impacts approximately eight million people across the United Kingdom, is now at the centre of urgent calls for systematic workplace screening programmes.
The Economic Impact of Undiagnosed Sleep Disorders
According to a comprehensive study conducted by experts from both the UK and United States, analysing data from the 2021 census, the economic consequences of untreated OSA are profound. Researchers calculated that among working-age adults between 18 and 64 years old, productivity losses reach up to £4.22 billion annually, equating to approximately £1,840 per affected worker each year.
The study revealed that around 7 percent of working-age individuals in the UK data met the clinical criteria for obstructive sleep apnoea. This condition occurs when throat walls relax, narrow, or completely close during sleep, resulting in symptoms including loud snoring, choking noises, and frequent nighttime awakenings. These disruptions lead to severe daytime fatigue, concentration difficulties, and mood disturbances that directly impair workplace performance.
Call for Workplace Screening Initiatives
Researchers are now advocating for the implementation of pilot screening schemes, particularly targeting occupations where daytime sleepiness presents heightened safety risks. Professional driving roles have been specifically highlighted as a priority area for initial trials, given the potentially catastrophic consequences of impaired alertness in these positions.
"Given the significant yet often-overlooked burden of OSA syndrome and its substantial economic impact, we urge policymakers to allocate resources towards developing an effective screening strategy," the research team stated. They emphasised that early identification and appropriate treatment could generate "substantial savings" for both employers and the broader economy.
Current Guidelines and Treatment Challenges
Existing National Institute for Health and Care Excellence guidance already recommends rapid assessment for OSA among drivers, train operators, pilots, and surgeons. However, researchers note there remains "limited data about occupational consequences of OSA" within these specific professions, highlighting the need for more comprehensive workplace studies.
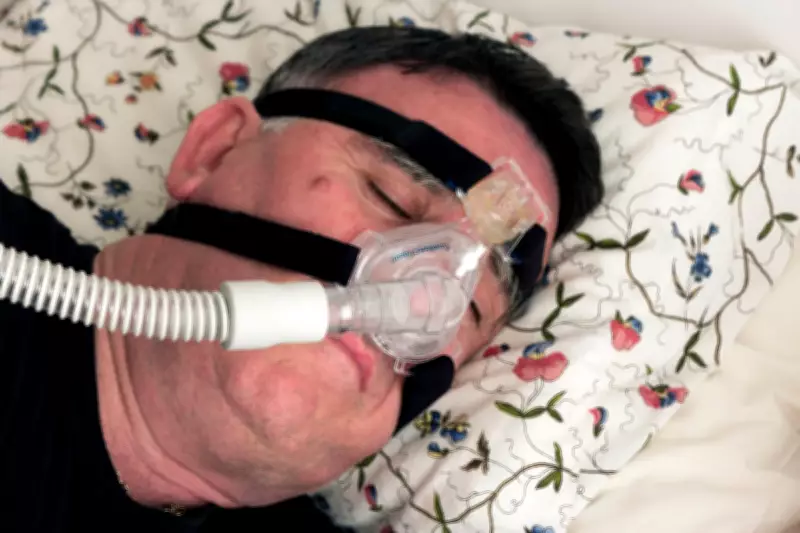
Alarmingly, approximately 85 percent of individuals with obstructive sleep apnoea in the UK currently remain undiagnosed, representing a massive hidden burden on workplace productivity and individual wellbeing. The primary treatment involves continuous positive airway pressure (Cpap) machines, which deliver pressurised air through a mask during sleep, though many patients find these devices uncomfortable.
New Treatment Options and Implementation Considerations
Recent medical advances offer promising alternatives, including the GLP-1 receptor agonist tirzepatide (marketed as Mounjaro), recently approved in the United States for obese patients with moderate to severe OSA. Researchers noted that "treatment options for individuals with OSA are also improving with better Cpap adherence interventions on the horizon and new non-Cpap therapies."
The research team acknowledged potential worker concerns about employment repercussions if they cannot tolerate treatment, suggesting that any successful screening programme should incorporate employment guarantees. "We suggest the time is now approaching for a trial of workplace screening in an exemplar high-risk occupational group," they concluded.
Industry and Union Responses
The Sleep Apnoea Trust welcomed consideration of screening programmes while cautioning that "it is very important that workplaces support their employees by not penalising them if they come forward." The organisation emphasised the need for employers to make necessary adjustments during clinical diagnosis and treatment processes.
Adrian Jones, national officer at workers' union Unite, highlighted the particular concerns among professional drivers: "Professional drivers often hide issues of sleep apnoea out of fear of losing their jobs. Before introducing screening, employers must be fully educated that sleep apnoea can be effectively managed. Workers must have the confidence that they will be supported not dismissed if a problem is identified."
Researchers proposed that the effectiveness of workplace screening could be tested by selecting an occupation with high OSA prevalence and severe potential consequences, such as professional driving, and comparing outcomes like road traffic accidents and absenteeism between screened groups and those receiving standard care.









