NHS Organ Preservation Pilot Could Boost Transplants by Hundreds Annually
A groundbreaking pilot scheme by NHS doctors could see hundreds more organs become available for transplant each year, potentially saving countless lives across England. The initiative focuses on extending the preservation time for donor organs through advanced perfusion techniques.
Addressing Critical Time Constraints
The pilot, currently underway in several major English hospitals, addresses a crucial challenge in transplantation medicine. Under current systems, doctors often lack sufficient time to conduct comprehensive checks on donor organs, leading to many being deemed unsuitable for transplant operations. This new approach provides that vital extra window for assessment.
Should the pilot prove successful, it would pave the way for the world's first national network dedicated to reconditioning organs. This could result in an additional 750 organ transplants annually, marking a significant 19 per cent increase on current figures. Specifically, this includes the potential for up to 202 more liver transplants, 202 more lung transplants, and 345 additional kidney transplants.
How Perfusion Technology Works
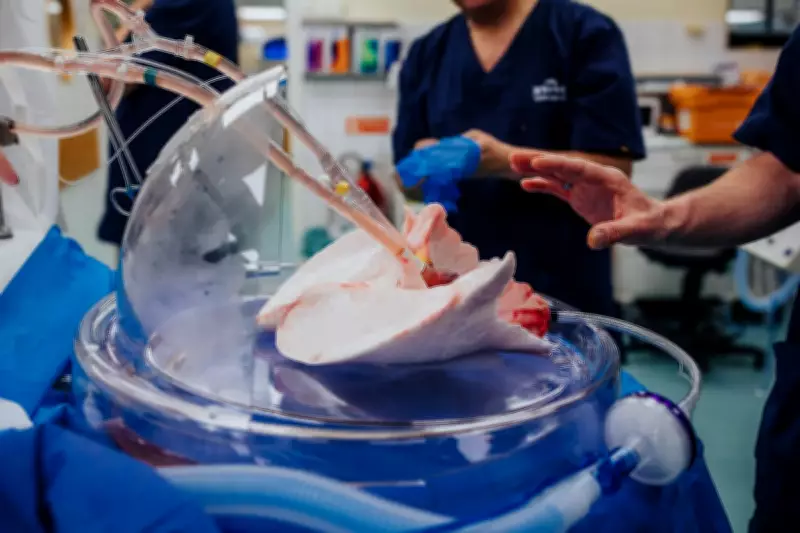
Perfusion is a technique for circulating oxygenated blood or nutrient-rich fluids through organs, preserving their function and enabling more time for them to be assessed. With this method, organs are connected to a device by tubes going into the arteries, then fed blood or an oxygenated substance plus nutrients while waste products are removed.
Derek Manas, medical director for organ and tissue donation and transplantation at NHS Blood and Transplant (NHSBT), explained the dual benefits: "One is to extend the preservation time. What the perfusion machines will do is give us more time to keep the organs viable. The other value of perfusion is assessing the functionality of the organs."
Expanding Preservation Windows
The extension of preservation times varies by organ type. For hearts, perfusion could extend viability from about three hours on ice to eight hours or longer. For livers, preservation could potentially extend to 12 to 24 hours. This additional time allows for better coordination of surgical teams, theatre availability, and comprehensive organ assessment.
The first lung pilot centre has opened at Royal Papworth Hospital in Cambridge, with additional lung pilot sites planned at the Freeman Hospital in Newcastle and Harefield Hospital in London. Some 12 liver and kidney pilot centres will also open in the coming months across multiple NHS trusts.
Addressing Growing Need
NHSBT says changes are urgently needed to save more organs owing to the record high transplant waiting list, which consistently exceeds 8,000 people. The potential donor pool is also falling as people live longer and develop long-term health conditions.
Anthony Clarkson, NHSBT director of organ and tissue donation and transplantation, emphasized the urgency: "Survival on the transplant waitlist is a daily struggle, and hundreds of patients will die this year before they can receive a life-saving transplant. Donation alone cannot close the gap."
Creating National Standards
While some NHS trusts already employ perfusion techniques, the pilot aims to standardize practice and create a national network. Manas noted the current inequity: "It's hugely inequitable at the moment, because some patients are getting the benefit and others are not. The pilot will hopefully change that."
With a full reconditioning network, organs could receive additional treatments such as surgical repairs, medications, blood group changing, or cell therapies, further increasing their suitability for transplantation.
Government Support and Future Vision
Dr Zubir Ahmed, the government's health innovation and safety minister, expressed strong support: "Every person waiting for a transplant deserves the best possible chance of receiving one. This programme could mean saving and transforming hundreds of lives that might otherwise have been lost."
The transplant centres acting as pilot sites include Cambridge, Newcastle, Oxford, Edinburgh, Royal Free, Manchester, and Hammersmith for kidneys; Cambridge, Royal Free, Kings College, Edinburgh, and Newcastle for livers; and Cambridge, Newcastle, and Harefield for lungs.
This innovative approach represents a significant step forward in transplantation medicine, potentially transforming outcomes for thousands of patients awaiting life-saving operations across England.









