Zimbabwe Pioneers Twice-Yearly HIV Prevention Drug for High-Risk Groups
In a significant public health development, Zimbabwe has emerged as one of the world's first countries to roll out lenacapavir, a groundbreaking long-acting HIV prevention drug that requires administration only twice a year. This initiative marks a pivotal moment in the nation's ongoing battle against an epidemic that has claimed tens of thousands of lives over the past two decades.
A New Dawn for Prevention Strategies
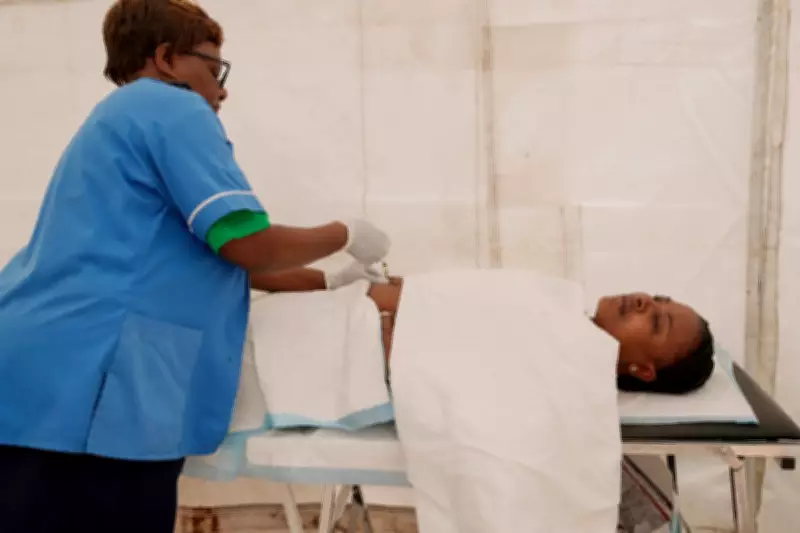
On the outskirts of Harare, Zimbabwe's capital, a diverse group including young women, mothers with infants, and men gathered in a dusty field. They were queuing for injections of this innovative drug, launched nationally on a recent Thursday. Clinical studies have demonstrated that lenacapavir offers near-total protection against HIV, leading health officials to describe it as a potential turning point, especially for high-risk demographics.
Constance Mukoloka, a 27-year-old sex worker, was among the first recipients. After receiving her dose from a mobile clinic, she expressed profound relief. "I am safe, I can work with confidence now," she stated, highlighting the practical challenges of daily oral preexposure prophylaxis (PrEP) pills, which often created tension with clients and were difficult to adhere to consistently.
Overcoming Stigma and Adherence Barriers
For individuals like Mukoloka, lenacapavir represents more than mere convenience; it addresses deep-seated stigma. "When I took tablets, customers would see a container of pills and leave. They would never return due to fear," she explained. "They couldn't tell the difference between PrEP and treatment drugs. With the work we do, that stigma costs you money."
While daily oral PrEP, condoms, vaginal rings, and shorter-acting injectables have long been available in Zimbabwe, adherence remains a persistent challenge. Factors such as social stigma, unpredictable schedules, and client resistance often undermine consistent use. Mukoloka recounted instances where work in beer halls, intoxication, or overnight shifts led to forgotten doses, increasing vulnerability.
Strategic Advantages and Broader Rollout
Health authorities emphasize that lenacapavir's discreet nature and extended duration offer critical advantages for key populations, including sex workers, adolescent girls, young women, gay men, and pregnant or breastfeeding women. Zimbabwe's Health Minister, Douglas Mombeshora, underscored this at the launch event: "Prevention must fit into real life. If a health solution is too complicated, too demanding, or too visible, people simply won't use it. Lenacapavir represents a new way of doing things."
The drug is being introduced in Zimbabwe as part of a donor-supported rollout across ten African nations, backed by the United States President's Emergency Plan for AIDS Relief (PEPFAR) and the Global Fund, in partnership with Gilead Sciences, the California-based developer. Similar initiatives have commenced in other southern African countries like Zambia and Eswatini.
Persistent Challenges and Demographic Disparities
Despite Zimbabwe, Eswatini, and Zambia making strides as global models in controlling HIV—achieving World Health Organization targets for testing, treatment, and viral suppression—new infections remain a concern. Adolescent girls and young women are particularly vulnerable. According to UN data, HIV prevalence in this demographic across sub-Saharan Africa is persistently triple that of their male counterparts, driven by gender inequality, poverty, and uneven healthcare access.
In the early phase, approximately 46,000 people across 24 sites in Zimbabwe are expected to benefit from lenacapavir, though this is only a fraction of the potential demand in a country of about 15 million. The government aims to expand access as more donor-funded doses arrive and eventually acquire its own supplies for a mass rollout, but financial constraints pose a significant hurdle.
Financial and Logistical Hurdles
The high cost of mass rollouts presents a formidable challenge across Africa, a continent with over 1.5 billion people. In Kenya, which recently received its first 21,000 doses, the negotiated price is about $54 per person annually—a substantial burden for many. While Gilead Sciences has committed to selling the drug at no profit to low- and middle-income countries heavily affected by HIV, experts warn that this alone is insufficient.
Bellinda Thibela of Health GAP, an international advocacy organization, noted that reduced pricing must be coupled with robust healthcare infrastructure. "What's the point of having a reduced price if there is no staff and equipment in clinics?" she questioned, highlighting the continent's heavy reliance on diminishing external funding, exacerbated by past foreign aid cuts.
A Complementary Tool in Prevention
Healthcare professionals stress that lenacapavir should complement, not replace, existing prevention methods. Enerst Chikwati, Zimbabwe program director at the AIDS Healthcare Foundation, emphasized: "Condoms remain key. They are cheap and they also prevent other sexually transmitted infections."
Nevertheless, for early recipients like Constance Mukoloka, the impact is already transformative. "I am elated. I can go for a whole six months feeling safe," she shared, encapsulating the hope that this new drug brings to those at highest risk in Zimbabwe and beyond.









